
Are You Ready to Apply to Med School? 6 Questions Before You Submit
Are you ready to apply to medical school? Use these 6 questions to assess your GPA, MCAT, clinical hours, and application strategy before you submit.

In a future doctor’s life, there are few decisions as important and nerve-racking as deciding on a specialty. Everything from your life during medical school to your life in residency to your life beyond residency are all dramatically influenced by this singular decision. How much money will you make? How much time will you have for your family? Will you be burned out and miserable or love what you’re doing?
We’ll cover the thought processes and practices you should go through to ultimately land on a specialty that is best suited for you. But an important part of the decision process is hearing from other doctors and learning what drew them to their field, what they love about it, and what they wish they did differently.
For that reason, we have a series called The Insiders Scoop, available exclusively here on the Med School Insiders blog, where we highlight individual doctors across various specialties. If you’d like to receive updates anytime a new specialty is featured, be sure to subscribe to our newsletter.

Data from a survey conducted by the AAMC on medical student specialty choice reveals that over the course of medical school, most medical students change their preferred specialty. Only a quarter (25-27%) of respondents indicated the same specialty between matriculating and graduating.
I can identify with that statistic. I initially started medical school wanting to go into pediatric gastroenterology. Ultimately, I switched to plastic surgery. I go over this journey and the process that led to my decision on my YouTube channel.
Interestingly, specialties that had the highest rate of congruence, meaning they did not change their specialty, included orthopedic surgery at 45.7%, pediatrics, and neurosurgery. I’m not quite sure what to make of those numbers. What do you guys think? Let me know in the comments below.
The specialty you decide on has tremendous immediate and long-term ramifications on your life. We also know that most medical students end up changing their mind over their four years in medical school. So where do we go from here, and how can we create a system to decide on the best suited specialty for ourselves?
Most commonly, people refer to compensation as a significant factor to help sway your decision. I don’t blame them, particularly when medical students graduate with well over $200,000 in debt.
Learn more in our article covering the Top Paid Specialties, which includes the factors that lead to certain specialties being highly compensated and others less so.
While compensation is important, I’d argue that most physicians are quite comfortable, and compensation differences between specialties will be far less important than other factors in helping you lead a happy and fulfilling life. Therefore, compensation should NOT be a primary or even secondary factor in making your decision.
Other, more important factors to consider include what type of relationship and interactions you want to have with your patients, the work-life balance you desire, how much or little you enjoy performing procedures, the types of patients you generally work with, and who your colleagues will be.
Does the specialty excite and captivate you? Can you imagine doing this for the rest of your life? Oftentimes, medical students fixate on rare cases or procedures that are particularly exciting in their field. However, it’s important to remember that these zebra cases are few and far between. More importantly, determine whether or not doing the bread and butter, meaning the things you are more likely to see day after day, is something you can live with, and, ideally, enjoy.
We’ll now cover a systematic approach to help you narrow down a category or group of specialties for you to deliberate on.
First, what organ system or clinical questions do you find the most exciting and stimulating? If you enjoy pharmacology and physiology, anesthesia may be a good fit for you. If you love anatomy, like I did, then consider a surgical specialty. If you are fascinated by the brain and how it works, then neurology or neurosurgery are appropriate considerations.
Next, assuming you plan to practice clinically, do you want direct patient care or indirect patient care? Indirect patient care includes specialties like radiology or pathology. Direct patient care includes most everything else.
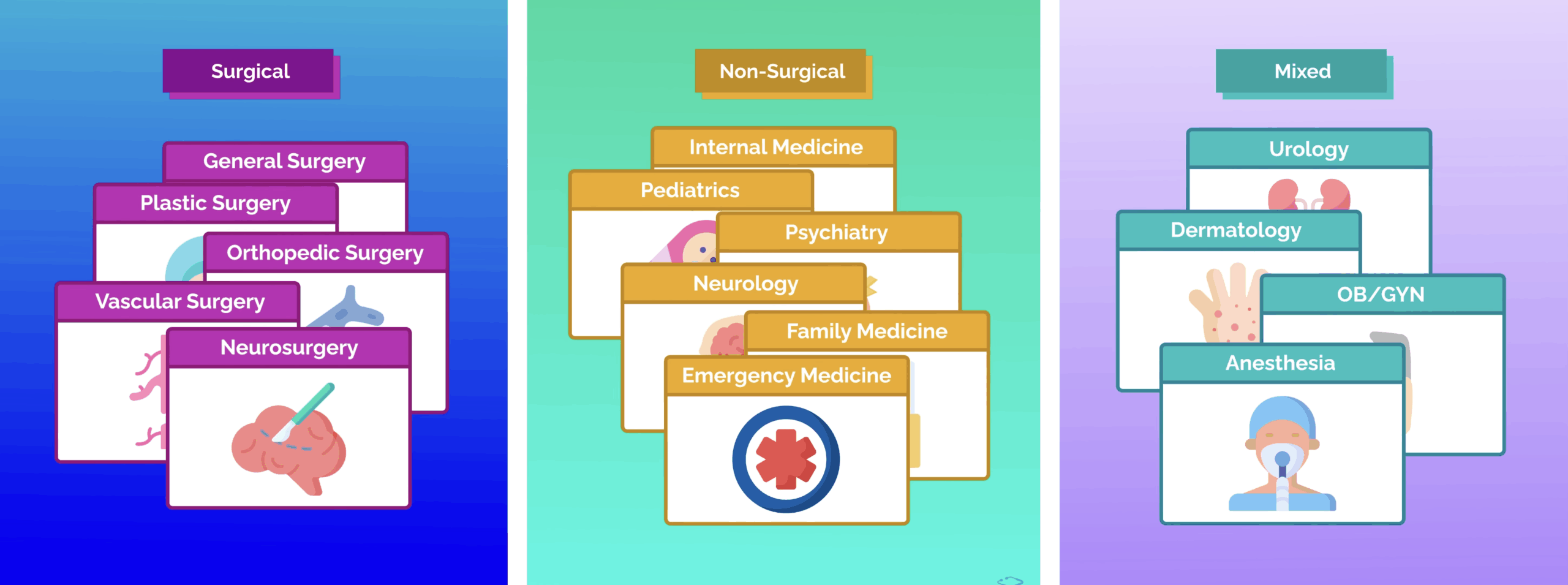
Next, assuming you want to have direct patient care, determine whether you’d like a primarily surgical practice, where the operating room is the focus of your day-to-day, or a primarily medical practice, where procedures are relatively rare.
Surgical specialty examples include general surgery, plastic surgery, orthopedic surgery, and the like. Medical specialties include internal medicine, pediatrics, psychiatry, family medicine, and other less procedurally-focused specialties. On average, these specialties emphasize patient relationships and clinical reasoning, but they often require a high degree of patience. You can also opt for a middle ground, like urology, dermatology, OB/GYN, or anesthesia, which allow for a mix of both.
Another important consideration when answering this question is the level of patient contact and continuity that you prefer. Do you enjoy talking to patients and forming long-term relationships? If so, internal and family medicine provide ample opportunity. Or do you prefer brief and efficient patient interactions? Emergency medicine, anesthesiology, and many surgical specialties are better suited for this preference.
When I first started medical school, I remember thinking that work-life balance wasn’t important. This is a common sentiment amongst premed and medical students. However, by the time you reach the end of medical school and have been put through the wringer, you begin to realize how important your lifestyle is.
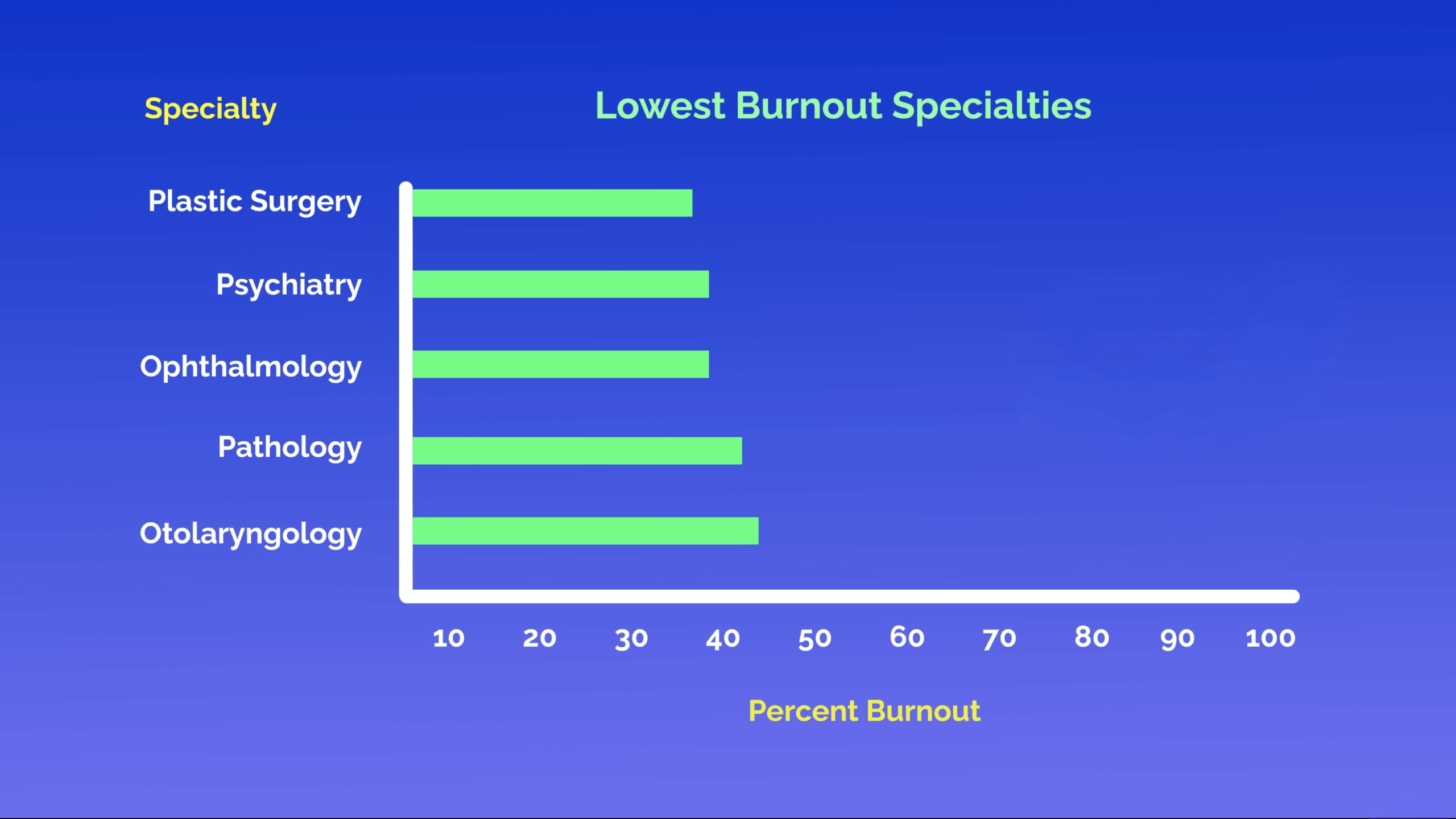
It’s easy to simply correlate challenging or unpredictable work hours with higher rates of burnout, but it’s more complicated than that. On average, surgical specialties have much more challenging hours than non-surgical specialties, but the burnout rates are not necessarily higher in surgical specialties.
The 2019 Medscape National Physician Burnout, Depression, & Suicide Report provides data on the burnout rates across various specialties. The highest rates of burnout are found in urology at 54%, neurology at 53%, physical medicine & rehabilitation at 52%, internal medicine at 49%, and emergency medicine at 48%. The lowest rates of burnout were found in public health & preventive medicine at 28%, nephrology at 32%, pathology at 33%, ophthalmology at 34%, and otolaryngology and plastic surgery at 36%.
Factors that were cited as most contributory to burnout include too many bureaucratic tasks, such as charting and paperwork at 59%, spending too many hours at work at 34%, and increasing computerization of clinical practice at 32%.
An often understated yet highly important factor is determining the type of patients and the outcomes you are most comfortable with. Entering my surgical rotations, I felt drawn to neurosurgery given my interest in anatomy and love for neuroscience, which I majored in. However, the surprising lack of precision in neurosurgery, but more importantly, the poor outcomes of neurosurgery patients, turned me off from the specialty.
Consider the typical patients you will encounter in your specialty of choice. The types of patients and interactions emergency physicians face on a daily basis is far different from what the average pediatrician or orthopedic surgeon faces.
Lastly, there are a few considerations you should keep in mind, although these will likely not be as important as those previously mentioned.
First, assess your own skills. While most skills can be learned, there’s also some benefit to playing to your strengths. On average, we enjoy things we’re good at. If you’re a klutz and particularly uncoordinated, then procedural-focused specialties may not be a good fit.
Second, consider the competitiveness of a specialty. If you’re barely managing to get by in medical school, then the chances of you matching into something like plastic surgery may be relatively slim. That being said, I’m a firm believer that the majority of one’s performance in college or medical school is dictated by their study strategies, habits, and systems.
If you’re struggling in college or medical school, our team of exceptionally qualified and effective tutors can help you turn things around. We stand for results at Med School Insiders, and our tutoring is a perfect example of this.
Third, consider what type of activities you’d like to engage in outside of clinical practice. Are you interested in research, teaching, or policy work? In most cases, this preference is more important in determining your practice type, meaning private practice vs. academic vs. community, rather than your specialty choice.
Addressing the previously mentioned questions should do a good job in narrowing down your specialty of choice. You now likely have only a handful of specialties that you’re considering. Prior to pulling the trigger and committing to one, however, it’s essential that you get clinical exposure.
If it wasn’t for gaining clinical experience, I would not have realized that gastroenterology was not a good fit for me. Make sure you shadow attending physicians in your areas of interest as much as possible. Specialty clubs and talks from physicians across various specialties are also a great way to gain exposure to different specialties. Our series, The Insiders Scoop, is another great way to gain insight in a particular specialty.
Once you’ve decided, the next step is making sure you match into a desirable residency program in your specialty of choice. For this reason, it’s essential that you make your residency program application as authentic as possible. Don’t fall into the trap of researching a specialty and finding one you love, only to submit a residency application that sounds similar to your colleagues. The personal statement, letters of recommendation, and soft parts of your application are just as important as your test scores.
Maximize your chance of acceptance with our Residency Admissions Consulting Services. Our advisors are physicians with extensive experience on admissions committees at top programs across the nation.

Are you ready to apply to medical school? Use these 6 questions to assess your GPA, MCAT, clinical hours, and application strategy before you submit.

Medical school secondary questions follow predictable patterns. Here are 11 of the most common prompts and how to answer them effectively.