
How Many Times Can You Apply to Medical School?
How many times can you apply to medical school? Learn the limits, what’s actually advisable, and what to do if medicine doesn’t work out.
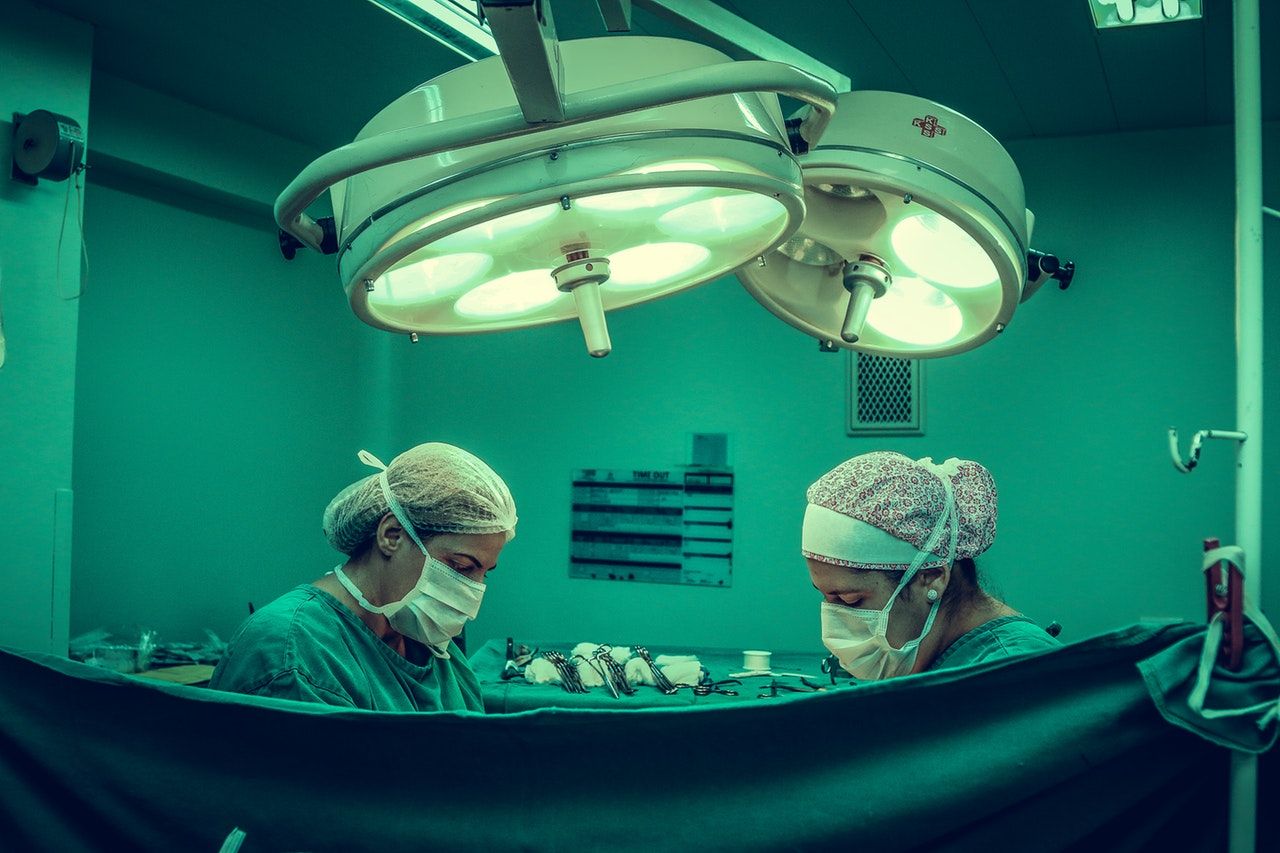
Welcome to our second installment in the So You Want to Be series: So You Want to Be a SURGEON. In this series, we highlight a specific specialty or type of professional within healthcare, explaining not only what it means to be that type of provider, but also how to become one. If you want to help us decide which specialty or healthcare professional to cover next, drop a comment down below with your request.
If you’re thinking of becoming a surgeon and want to know what it would entail and if you’d like it, this post is for you. I’ll take you through the history, types, and duties of a surgeon, to help you decide if it would be a good fit for you!
There are several stereotypes of surgeons, one of them being that they love history. So pay attention. The history of surgery is a fascinating story, and my medical school actually provided us with a copy of An Anatomy of Addiction to read prior to starting our first year. It’s one of my favorite medical books, covering Dr. William Halsted and the birth of modern surgery, and if you’re interested in any surgical specialty, definitely check it out.
Until the 19th century, surgeons were trained simply by apprenticeships – there weren’t formal residency programs as there are today. The length of training could vary, usually lasting anywhere from 5 to 7 years and starting around the age of 12 or 13. That’s right, imagine a tweenie cutting you open and be grateful that you live in the 21st century.
In the 1890’s, Dr. William Osler of Johns Hopkins introduced the concept of clinical clerkships and bedside rounds to teach his medical students, which are now the norm today. In the early 1900’s, Dr. William Halsted moved to Baltimore and was appointed the first chief of the department of surgery at Johns Hopkins. The modern practice and training of surgery can be largely attributed to the anal-retentive, cocaine-addicted, and incredibly badass Dr. Halsted.
He not only created the first formal surgical residency training program in the U.S. at Johns Hopkins, but also pioneered many other aspects of modern surgery that we take for granted today. His advances resulted in new techniques and instruments to reduce damage to tissues and blood vessels, such as different types of forceps, suture, and ligatures. He was also the first to introduce rubber gloves to the operating room and was the father of modern sanitization in surgery. We call many of his lasting impressions Halsted’s principles, including modern techniques for hemostasis (meaning the control of bleeding), accurate anatomical dissection, complete sterility, and gentle handling of tissues. If you’ve ever had surgery, or even a small procedure using local anesthetic, you can thank Dr. Halsted for it not being a barbaric mess.
There’s a wide spectrum of surgical subspecialties, and it isn’t fully agreed upon what being a surgeon entails. Let’s start with the most traditional forms of surgery.
The core is of course general surgery, originally being the broadest category of surgery. However, over the decades, it has mostly been relegated to procedures of the gastrointestinal, meaning digestive, and endocrine systems. In medical school and residency, we joke that general surgeons are the true masochists, as their lifestyle is nothing to be envious of, they don’t make as high of salaries as other specialists, and they handle some of the less desirable and odorous pathologies dealing with abdominal contents and fecal matter. In all seriousness, it’s a pretty awesome specialty and I know some great general surgeons, like Dr. David Hindin who provided me some insights about general surgery when making this post. Be sure to check out his channel on YouTube.
General surgery residency is 5 years, after which you can specialize further. Colorectal surgery is a 1 year fellowship, dealing with pathologies such as colon cancer or inflammatory bowel disease. Minimally invasive surgery is also a one year fellowship, and focuses on techniques like laparoscopic surgery that are less invasive than the traditional open abdominal procedures. Transplant surgery is 1-2 years, and focuses on kidney and liver transplants most commonly, but also pancreas transplants and access procedures such as dialysis fistulas and peritoneal dialysis catheters. Surgical critical care is 1 year, focusing on patients who are more medically unstable and requiring acute surgical interventions. Pediatric surgery is 1-2 years, obviously focusing on surgery in babies and children. Vascular surgery is also a 1-2 year fellowship, dealing with procedures of the aorta, carotid arteries, varicose veins, dialysis access, or other procedures dealing with arteries and veins.
Surgical oncology is 1 year, dealing with cancer pathologies, meaning the resection, or removal, of the tumor. Breast surgery is 1 year, focusing on breast cancer and other breast pathologies. Surgical oncologists and breast surgeons remove the tumor, but don’t cover the defect themselves. They turn to plastic surgeons for complex coverage and reconstruction. Plastic surgery is moving toward an integrated residency, meaning 6 years of dedicated plastic surgery training after medical school. However, there are some more traditional independent pathways, meaning 3 years of plastic surgery fellowship after completing 5 years of general surgery. Cardiothoracic surgery is 2-3 years, focusing on surgery of the heart and thoracic cavity, although there is also an integrated pathway, which, similar to the integrated plastic surgery route, is 6 years. Hand surgery is a 1 year fellowship, although only a few percent of practicing hand surgeons take this route after general surgery. Over 90% of hand surgeons have completed an orthopedic surgery or plastic surgery residency first, and then take the 1 year fellowship. This was the path I was intending to take after completing my plastic surgery residency, but I said YOLO and resigned in 2018.
There are other fields that perform surgical procedures, but some surgeons wouldn’t call it surgery in the traditional sense. OB-GYN doctors perform procedures like Cesarean sections, which is less refined, way more crude, and far less complex than regular surgery. That being said, OB-GYN doctors also do hysterectomies, meaning surgical removal of the uterus, and other gynecology oncology resections that certainly count as surgery. The other surgical specialty that isn’t really surgery is ophthalmology. We generally consider ophtho to be more of a procedural specialty than a surgical subspecialty.
Entering medical school, surgery really wasn’t on my radar. I was enamored with the idea of being a gastroenterologist and helping pediatric patients that have inflammatory bowel disease and similar pathologies. I’ve always known that I wanted to work with my hands, as it’s something that comes naturally to me and I greatly enjoy it, but I soon realized that the procedures of gastroenterology aren’t as complex, nuanced, or varied as I would like. I couldn’t imagine myself doing scopes for the rest of my career. The procedural complexity and excitement in surgery, on the other hand, is second to none. After seeing my first case, a joint neurosurgery and plastic surgery case where we created a makeshift bicep out of someone’s latissimus dorsi, I was hooked. I couldn’t believe this was real life and not science fiction. If you want to hear the full story, I talk about why I chose plastic surgery, including that amazing first case I saw, on my Kevin Jubbal, M.D. YouTube channel.
If you enjoy working with your hands and enjoy complexity, challenge, and nuance, surgery may be a good fit for you. Other specialties may include procedures, like endoscopies in gastroenterology or skin excisions in dermatology, but they are certainly not anything like surgery. Comparing these simple procedures to surgery is like comparing driving automatic with paddle shifters to a true manual transmission car. Not that one is better than the other. It’s just not really a comparison.
Another point that comes up is one’s dexterity. After all, surgeons need to be incredibly dextrous to perform at the highest level. There are two things to say about this. First, having terrible dexterity and being incredibly clumsy has been a limiting factor in some people being able to complete residency, but it is quite rare. For most, they are able to learn how to be more efficient and effective with their hands and surgical instruments. That being said, being dextrous and working at it deliberately years before you first enter an operating room will serve you well. I credit much of my own dexterity to building small model cars as a kid, pursuing artistic endeavors, and even playing video games. In medical school, I was highly disciplined about reading proper techniques for suturing, knot tying, and other basic procedures, and practiced religiously at home or even while listening in lecture. I would brush my teeth and open doors with my left hand, a habit I still practice to this day. This sort of dedication served me well, as attendings noticed I was operating several years past my training level. In fact, the chair at a highly prestigious plastic surgery residency even said I was operating at a second or third year resident level while I was a fourth year medical student. By demonstrating competence, you will earn the trust of attendings, and they will allow you to do more. Many medical students or interns complain about not being able to do much in the operating room. I tell them it’s probably because they haven’t developed the skills to warrant being able to do much beyond retracting. By working at my skills, just a few months into residency I was able to do my own half of a blepharoplasty, a challenging procedure usually reserved for higher level residents, as it involves highly precise operating on the eyelids, the thinnest skin in the human body.
Surgery is awesome, but being a surgeon is not without major costs. The main factor holding people back from choosing a surgical specialty is the lifestyle, meaning your work-life balance, or lack thereof. You’ll work harder than non-surgical physicians, which only makes sense. Not only do you have to round on your patients and handle them medically, but also handle them surgically which can take several hours for each case.
Within surgery, some subspecialties have more challenging and demanding lifestyles than others. Residency for just about any of the traditional surgical specialties is going to be very challenging. As an attending, however, the lifestyles are more variable. As a general rule, any surgical specialty where taking “call” with urgent medical conditions is going to result in a more challenging lifestyle. Not all “call” is created equal, as sometimes when you’re paged you need to come in immediately, and other times you can just wait until you come later in the morning. When I was rotating on a sub-internship on a burn service in plastic surgery, we paged the dermatologist at 3AM for ruling out a life threatening condition, but she only showed up at 6AM. Dermatologists simply aren’t used to life or death situations. On the other hand, trauma surgeons and neurosurgeons have the most challenging lifestyles, as their call includes emergency situations requiring a rapid response. Other surgical specialties with more demanding call schedules include general surgery, cardiothoracic surgery, and vascular surgery. Orthopedic surgery call isn’t that bad, unless you specialize in orthopedic trauma. Plastic surgery call isn’t that bad either, unless you specialize in microsurgery. We’ll be covering these subspecialties in greater detail in future So You Want to Be articles. If you’d like to be notified, be sure to sign up for our newsletter!
This may not be all that intimidating to you right now. When I was in college, I actively despised sleep, since it felt like a waste of time, and I wouldn’t think twice about having any issues with a challenging lifestyle. Truth is, the demanding lifestyle of surgery impacts everyone, no matter how efficient or dedicated or high energy you are. Pushing yourself to the limit day after day, year after year, is not the healthiest or most sustainable way to live. If you ever decide to have a family, or want to travel and pursue other time consuming hobbies, there’s obviously an impact there as well. For that reason, most surgeons say only choose surgery if you cannot see yourself doing anything else. The cost of becoming a surgeon is simply so high.
Are you interested in becoming a surgeon? If so, let us know down below what’s driving you, and what type of surgeon do you want to be?

How many times can you apply to medical school? Learn the limits, what’s actually advisable, and what to do if medicine doesn’t work out.
We’re ranking all 22 specialties by the percentage of positions filled by US MD seniors. This is lowest to highest fill rate for US MD seniors, starting with the most accessible specialties up to the hardest.
This Post Has 2 Comments
I am a CNA working in the ER and find being a trama surgeon interesting in almost done with high school and I work a lot of OnCall hours.
Hi! I’m a cna as well and i’m looking into becoming a trauma surgeon as well. i’m currently in medsurg. did you pursue trauma surgeon?