
Are You Ready to Apply to Med School? 6 Questions Before You Submit
Are you ready to apply to medical school? Use these 6 questions to assess your GPA, MCAT, clinical hours, and application strategy before you submit.

AI is coming for your medical career. At least, that’s what everyone’s saying.
Algorithms will replace radiologists. Pathologists are obsolete. Even surgeons might get swapped out for robots. Every week, there’s another article about how artificial intelligence is about to make doctors irrelevant.
Med students are panicking. Premeds are second-guessing their entire life plan. And honestly, who can blame them?
But here’s the thing—while everyone’s busy worrying about AI taking over medicine, some doctor careers are more in demand now than ever before. And the specialties that are desperately needed right now will probably surprise you.
These are the most in-demand doctor careers.
Starting off the list is the 10th most in-demand specialty—radiology.
Here’s the irony of radiology. Everyone thinks radiologists will be the first to go when AI takes over, but right now, we’re facing a massive radiologist shortage.
Our aging population means more imaging studies than ever before. CT scans, MRIs, ultrasounds—the demand is through the roof. And despite all the AI hype, these algorithms still need human doctors to interpret their findings and make clinical decisions.

So in reality, at this present moment, AI is actually creating more work for radiologists, not less. Someone needs to review the AI-flagged abnormalities, correlate the findings with the patient’s history, and communicate the results to the referring physicians.
That said, medical technology is advancing more rapidly than ever before. What’s in demand today may be completely different five years from now. If radiologists become 10 times more efficient due to AI, the demand for these physicians will likely decrease significantly in the near future. To know more about the potential of AI to revolutionize healthcare careers, check out the video below.
Coming in at number 9 is anesthesiology. And here’s the thing about this specialty: Every single surgery needs an anesthesiologist. Every. Single. One.
With our aging population, surgical volumes are skyrocketing. Hip replacements, cardiac procedures, cancer surgeries—they all require expert anesthesia management. The increased demand is also rapidly driving up salaries.
Anesthesiologists’ pay increased by 14% from 2022 to 2023 and by an additional 6% from 2023 to 2024. In comparison, average physician salaries only increased by around 3% per year.
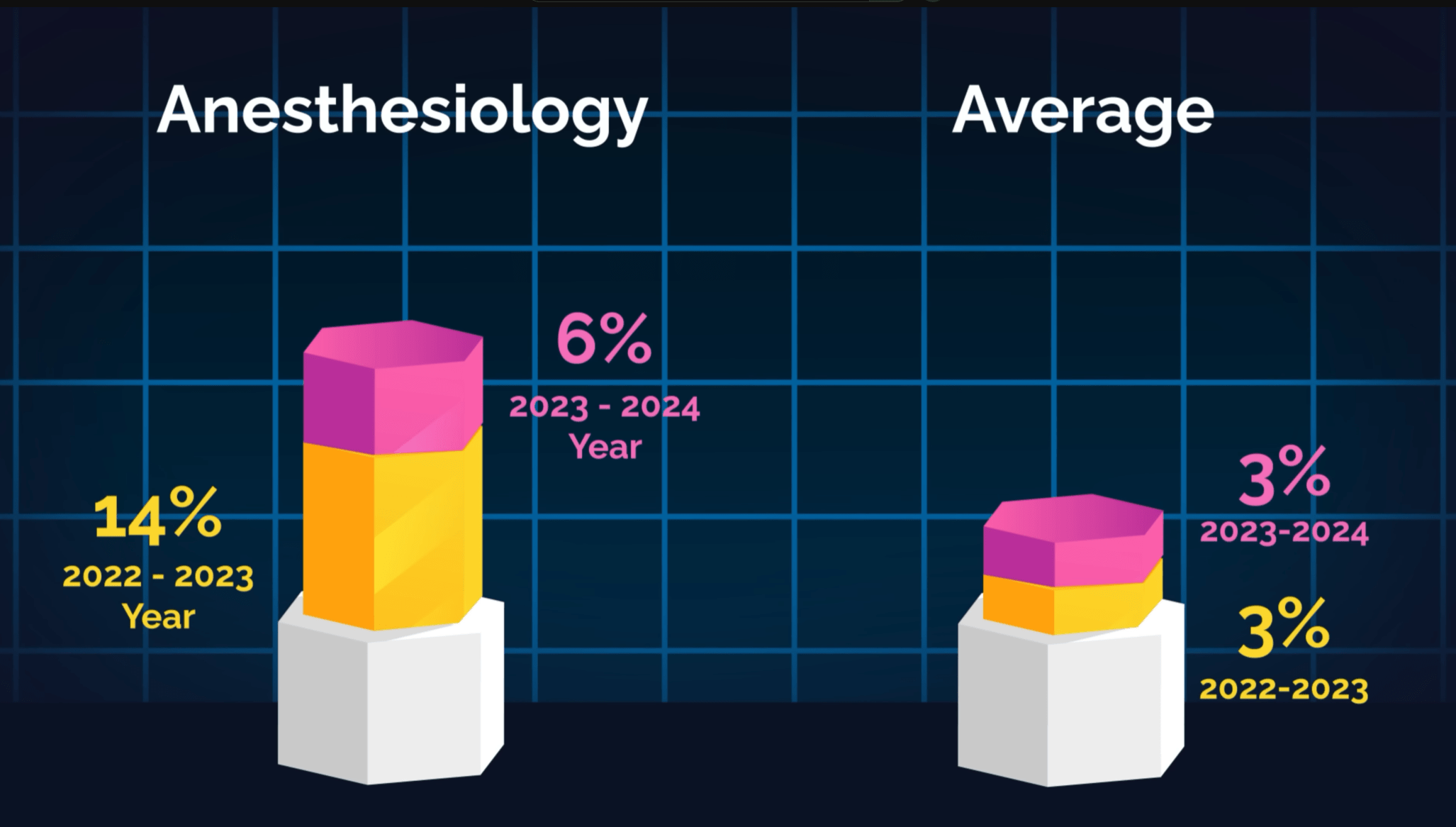
Rural areas are hit especially hard. Many hospitals are struggling to recruit anesthesiologists, which means CRNAs are filling in the gaps under the supervision of a “supervising MD.” This is foolish and incredibly dangerous for patients.
Consider the tragic case of Emmalyn Nguyen in Colorado. During a breast augmentation surgery, she went into cardiac arrest twice after being anesthetized by a CRNA. She slipped into a coma and died 14 months later. This case underscores the dangers of allowing CRNAs to administer anesthesia without direct oversight from an anesthesiologist.
Dr. Geoffrey Kim, the plastic surgeon and supervising MD, was charged with first-degree aggravated assault and criminally negligent homicide. The only supervising MD for a CRNA should be an anesthesiologist, not the surgeon.
At number 8 is general surgery, which serves as the foundation for all surgical subspecialties.
The lifestyle is brutal, composed of long hours, emergency calls, and high malpractice premiums. New medical graduates are increasingly choosing specialties with better work-life balance, resulting in a critical shortage in general surgery.

And once again, rural areas are being hit the hardest. This means patients have to travel hours for basic procedures like appendectomies, meaning removal of the appendix, or cholecystectomies, meaning removal of the gallbladder.
What people don’t realize is that general surgeons are essential to trauma centers. When someone comes into the ED with a life-threatening injury, you need a general surgeon or a trauma surgeon available 24/7.
There’s no substitute for that expertise. While it may not be as glamorous as other surgical fields, general surgeons are in high demand.
Next, at number 7, we have neurology.
Our aging population is leading to more cases of neurological disease than ever before. Stroke rates are climbing. Alzheimer’s and other dementia cases are projected to triple by 2050, and Parkinson’s disease is on the rise as well.
Right now, patients are waiting months to see a neurologist. The wait times are absurd, and it’s only getting worse.
The pipeline of new neurologists isn’t keeping up with demand. Medical schools graduate plenty of students, but the number of neurology residency spots remains limited compared to the growing need. That means outstanding job security for those who choose neurology, but it’s a serious problem for patients struggling to access care.

At number 6 is emergency medicine.
Emergency departments are the safety net of American healthcare. No matter what happens, whether it’s a pandemic, natural disaster, or mass casualty event, EDs have to stay open 24/7.
But we’re seeing a mass exodus from emergency medicine. The COVID pandemic overwhelmed many ER doctors. Burnout rates are skyrocketing, and many experienced physicians are leaving the specialty altogether.
Rural EDs are closing at an alarming rate, creating healthcare deserts where the nearest emergency care is hours away. And with the ongoing mental health crisis, ED visits are increasing while the number of available doctors is decreasing.

Interestingly, emergency medicine has become less competitive to match into in recent years—not because it’s less critical, but because fewer students want to deal with the lifestyle challenges.
Before we continue with our list, here’s something critical to understand: being in demand doesn’t mean most competitive or hardest to match into. Emergency medicine ranks 6th on our most in-demand list, but it’s actually one of the least competitive specialties, ranking 20th out of 22.
When a specialty is in high demand, it’s usually for a reason, such as extreme working conditions, poor pay, high burnout, or increased charting. These factors deter students from pursuing these careers despite the desperate need, which actually makes them less competitive to match into.
When you’re trying to figure out which specialties you can realistically match into, you need actual data—not just what you heard from that one gunner in your class or someone’s hot take on Reddit.
I recommend checking out Specialtyranking.com because it takes all the NRMP specialties and ranks them by multiple competitiveness metrics: Step 2 scores, match rates, research requirements, and more. You can filter it based on what matters for your specific profile, and it’s completely free.
It’s just a straightforward way to get a reality check on where you stand without the speculation and anxiety that comes with trying to piece it together from unreliable sources.
Now back to our list. Coming in as the 5th most in-demand specialty is OB/GYN.
Unfortunately for patients, America has a maternal mortality crisis, and it’s getting worse.
We’re losing OB/GYNs faster than we can train them, especially in rural areas. Many counties have zero obstetricians, forcing pregnant women to drive hours for basic prenatal care or delivery.

The malpractice environment in OB/GYN is brutal. The lawsuits can be devastating, both financially and emotionally, which is driving doctors away from the specialty.
Recent policy changes around reproductive health are also affecting access to care in many states, creating even more demand for the OB/GYNs who remain in practice.
Despite being a moderately competitive specialty, there’s a real need for more OB/GYNs willing to serve diverse communities and handle high-risk cases.
At number 4 is pediatrics, and the 2025 match data tells the story: 147 out of 3,135 pediatrics spots went unfilled—that’s 4.7%, nearly double the 2.9% from 2023.
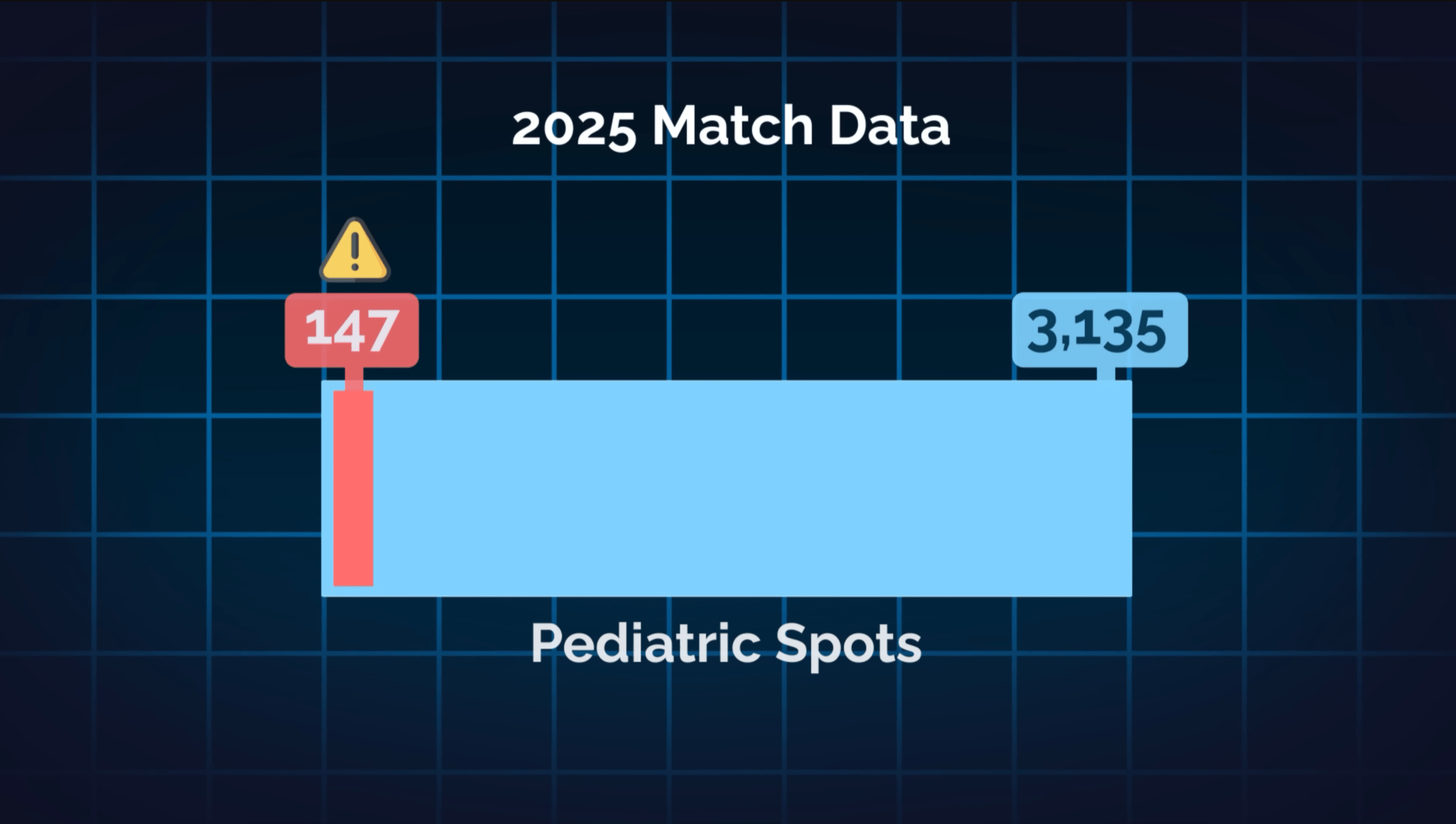
Children’s mental health is in crisis. The pandemic disrupted normal development for millions of kids, and pediatricians are on the front lines dealing with anxiety, depression, and behavioral issues they’ve never seen before.
Pediatric subspecialties are facing severe shortages. Child psychiatry, pediatric cardiology, and pediatric surgery all need doctors desperately, but the training is long, and the pay is often lower than in adult specialties.
The reimbursement rates for pediatrics are notoriously low compared to other specialties since children are more resilient and require fewer procedures than adults, and procedures are how hospitals make money. This makes the financial burden of medical school debt even more challenging for pediatricians to manage.
Rural areas are particularly affected. Many small towns have lost their only pediatrician, forcing families to travel long distances for basic child healthcare.
The 3rd-most in-demand specialty is psychiatry, which makes sense, considering that we’re in the middle of a mental health crisis that’s unlike anything we’ve seen before.
The stigma around mental health treatment is finally decreasing, which means more people are seeking help. That’s good news for patients, but it’s overwhelming the system.
Child and adolescent psychiatry is facing the most severe shortage. The wait times for kids to see a psychiatrist can be months, and in many areas, there simply aren’t any available.
The addiction crisis is creating additional demand for addiction psychiatrists who can handle complex cases involving opioids, alcohol, and other substances.

Despite the massive societal need, psychiatry remains less competitive than many other specialties, creating real opportunities for students who want to make a difference in mental healthcare.
This brings us to the runner-up for the most in-demand specialty: family medicine.
The 2025 data are stark: 805 out of 5,357 family medicine spots went unfilled—that’s 15%, more than triple the 4.3% from 2023.
Unfortunately, many med students look down on family medicine because it’s the least competitive specialty and the pay is near the bottom with pediatrics. It’s also a lot of primary care, which requires increased charting and admin now compared to the past.
However, there are many interesting and unique paths within the specialty, like sports medicine or concierge medicine. Check out the Day in the Life of a Concierge Medicine Doctor if you want to know more.
We’re facing a massive shortage of primary care physicians. Baby boomers are aging and need more complex medical management. Chronic conditions like diabetes, hypertension, and heart disease require ongoing care that only primary care doctors can provide effectively.
Rural healthcare access is becoming a real problem. Small towns are losing their family doctors, and there’s no one to replace them. As we already mentioned, this creates healthcare deserts where basic medical care is hours away.
Family medicine is consistently the least competitive specialty to match into, but it’s also the most desperately needed. The medical home model is increasing demand even further, as healthcare systems recognize the value of having a primary care physician coordinate all of a patient’s care.
And the number 1 most in-demand specialty? That goes to internal medicine, and the numbers prove it. In 2025, 357 out of 10,941 spots went unfilled—that’s 3.3% of the largest specialty by volume.
Our aging population has multiple chronic conditions that require expert management. Heart disease, diabetes, kidney disease, and COPD need internists who understand the complex interactions between different organ systems.

Hospital medicine is exploding as a field. More patients are staying in hospitals longer with more complex conditions, and they need internists who specialize in inpatient care.
Internal medicine also offers incredible flexibility. You can pursue primary care, specialize in cardiology or gastroenterology through fellowship training, focus on hospital medicine, or transition into administration or research.
The pandemic demonstrated the essential role internists play in managing critically ill patients and coordinating complex care during healthcare crises.
While AI headlines grab attention, human doctors are desperately needed right now. These unfilled residency spots represent incredible job security and opportunities to make a real difference in patients’ lives.
The specialties on this list aren’t just in-demand—they’re essential to keeping our healthcare system functioning. And despite all the talk about AI replacing doctors, these fields require human judgment, empathy, and complex decision-making that no algorithm can fully replicate—at least not yet.

Are you ready to apply to medical school? Use these 6 questions to assess your GPA, MCAT, clinical hours, and application strategy before you submit.

Medical school secondary questions follow predictable patterns. Here are 11 of the most common prompts and how to answer them effectively.