
Are You Ready to Apply to Med School? 6 Questions Before You Submit
Are you ready to apply to medical school? Use these 6 questions to assess your GPA, MCAT, clinical hours, and application strategy before you submit.

So you want to be an allergist/immunologist—working all day in an outpatient clinic taking care of runny noses. Let’s debunk the public perception myths and give it to you straight. This is the reality of allergy and immunology.
Welcome to our next installment in So You Want to Be. In this series, we highlight a specific specialty within medicine to help you decide if it’s a good fit for you. You can find the other specialties on our So You Want To Be blog category or YouTube playlist.
Allergy/immunology, often referred to as AI, is a specialty that cares for patients across the age spectrum who have misbehaving immune systems. AIs care for people with allergies, respiratory diseases like asthma and occupational lung disease, immune deficiencies, and certain types of autoimmune conditions.

They also play an important role in cancer, vaccine, and immunotherapy research. Immunotherapy, sometimes referred to as immuno-oncology, uses the body’s own immune system to prevent, manage, and eradicate cancer. Research is such an important aspect of the allergy and immunology field that some AIs choose to be research physicians who dedicate most or all of their time to lab work or clinical trials.
AI specialists enjoy reasonable hours and no shortage of patients or entrepreneurial opportunities, but they also must spend significant one-on-one time with patients.
Plus, the complex nature of the specialty means you must be committed to lifelong learning. No matter how much they know about the field, an AI can come across conditions no one has seen before. For some, this means the work always provides exciting puzzles to solve, but others may find the ever-evolving practice and influence of new AI technology overwhelming.
First, let’s break down the difference between academic, research, and private practice for AIs.
Academic AI physicians tend to work within a large hospital system associated with a medical school. Although most of the work is outpatient-based, you may be asked to weigh in on patients admitted to the hospital who have drug allergies or immune deficiencies. In addition to clinical duties, AIs are responsible for teaching residents and medical students.
Unlike many other specialists, AIs may choose to focus on research exclusively even though they are clinically trained. Research physicians often conduct their work in the lab or run clinical trials. Research-focused AIs might choose 100% research while others may have a 90/10 split. Most spend a 3rd year of fellowship devoted almost entirely to research if they are interested in this career path.
Both academic and research AI physicians typically focus on a particular area within the field, such as immune deficiency, asthma, chronic hives, or drug allergies.
Private practice AI physicians tend to spend nearly all their time in the outpatient office. Additionally, they’ll more often care for people with allergies and asthma. There is also a stronger focus on immunotherapy, like allergy shots and oral immunotherapy for food allergy treatment.
In a previous video, we covered the differences between academic vs community vs private practice.
Another differentiator is whether or not the AI sees pediatric or adult patients or some combination of both.
All AI physicians are cross-trained to care for both children and adults, whether their residency training was in pediatrics, internal medicine, or both. Each program has a minimum of 20% crossover training.
Community-focused AIs tend to have close to an even split between pediatric and adult patients.
Pediatric AI physicians will see patients from birth through young adulthood, caring for not only runny noses and asthma but also food allergies, eczema, eosinophilic esophagitis, and primary immune deficiency disorders.
Adult AI physicians will see teenagers and older. You will see more asthma, COPD, nasal polyps, chronic urticaria/angioedema (hives and swelling), and drug allergies in this patient population.
The reality is most allergists see both children and adults in their practices. Since allergic conditions are partly inherited, they often care for entire families. However, the more niche the practice, the more likely they are to specialize in one or the other. For instance, a food allergy practice might see almost entirely pediatric patients.
Let’s dispel some common misconceptions about the allergy/immunology specialty.
Many people say AI is boring because most of the physician’s time is spent in an outpatient clinic caring for runny noses all day. While this will likely take up some time, it’s far from all that’s involved.
The reality is the immune system is active in every single area of the body. This means allergists get to collaborate with physicians in every specialty of medicine, such as internal medicine, pediatrics, gastroenterology, pathology, and oncology. Additionally, they are always on the lookout for and ready to treat allergic emergencies like anaphylaxis—especially if they are treating patients with immunotherapy, such as allergy shots and similar treatments.
These complex patients also tend to be referred because no one else has been able to figure out the problem yet, which makes this type of work exciting for problem solvers, those committed to lifelong learning, and physicians who want to stay on the cutting edge of medicine.
To become an AI physician, you must first complete 4 years of medical school and then complete an internal medicine or pediatrics residency, which is 3 or 4 years in duration. After completing residency, a 2 to 3 year allergy & immunology fellowship is required.
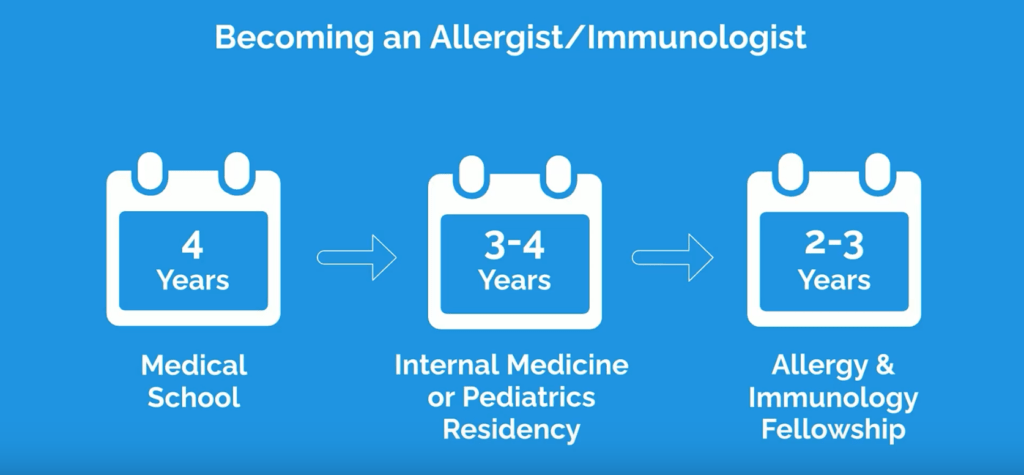
Programs vary in length depending on the amount of time devoted to research. Typically, longer 3-year programs will be especially helpful for those looking to have a career in research or academia. If you want to pursue community or private practice, 2-year fellowships may suffice, depending on the particular areas of the field you’re interested in.
Each program may have a different ratio of pediatric to adult care and immunology versus allergy. AI fellowships each have their own flavor. Certain programs will have a greater emphasis on food allergy treatment, drug allergy, immune deficiency, or other types of research.
Internal medicine, which allergy/immunology is a subspecialty of, is among the bottom 10 least competitive medical specialties. Our analysis puts internal medicine as the 9th least competitive specialty. However, if your goal is to match into a top-tier IM residency, you will still need to ace your Step exams and secure plenty of research experience.
The competitiveness of the AI subspecialty has fluctuated considerably in recent years but has seen an overall increase in competitiveness. 199 applicants applied for 154 positions in 2023. The most recent match data shows that only 3 spots remained unfilled. 82% of applicants matched to a fellowship spot.
Compared to other internal medicine subspecialties, allergy/immunology is toward the lower end of competitiveness, with cardiology, oncology, and gastroenterology being more competitive, and nephrology and infectious disease being less competitive.
The type of medical student who is typically drawn to AI tend to be those who are outgoing and enjoy working with many different types of people, including various physicians and pediatric and adult patients. AIs are often extremely curious and inquisitive people, as they work in a field with many unanswered questions.
Most AI doctors don’t pursue additional training after fellowship. However, for those who want to focus on a specific disease or area within allergy/immunology, that path is typically straightforward. The solution is usually to stay in academia and focus on your interests by learning from mentors and completing more research in that field.
For example, you can become the immune deficiency specialist or food allergy specialist at your institute. If you’re interested in Med/Peds, you can continue to care for patients with allergies, asthma, or immune deficiencies across lifespans.
Allergy/immunology offers a fantastic lifestyle with plenty of flexibility. Office hours are typically 8-5 with minimal overnight call responsibilities, even in academic centers. The flexibility of the specialty means many physicians continue practicing rather than retiring early.
The most famous immunologist, Dr. Anthony Fauci, love him or hate him, is known for being a leader in the medical community, his devotion to understanding the science of our immune system, and continuing to work into his 80s. He plays into the stereotype that AIs tend to continue practicing even with one foot in the grave. This is largely because the work is fun, not terribly taxing on the physical body, and you can always step back to part-time.
There’s also a good mix of academic and private practice opportunities for graduating fellows.
Although the bread and butter includes a lot of runny noses, you will have significant ability to tailor a practice to a particular niche, such as food allergy treatment or immune deficiency.
AI also allows for the kind of continuity of care and care within families that you might typically expect from primary care specialties. If you love people and are energized by the idea of forming lifelong relationships with your patients and their families, this is definitely a specialty to consider.
If you have an entrepreneurial spirit, AI offers many ways to make a good income for a non-surgical specialty, such as through allergy immunotherapy, infusion centers, and participation in clinical trials. Additionally, with climate change, lifestyle factors, and the ever-increasing rates of atopic and autoimmune diseases, you will have no shortage of patients in the coming decades.
Recent years have proven there is a significant need for immunologists. Successful physicians who take on leadership positions have the opportunity to help guide communities through evolving health crises and future pandemics.
AI is a primarily outpatient specialty. If you don’t like spending time talking with patients in the clinic setting, then this isn’t the specialty for you. It’s not a good fit for anyone looking for a procedure-heavy career. And if you’re looking for adrenaline-filled days, you won’t find it here though we always need to be prepared to identify and treat anaphylaxis!
However, you won’t fall into a boring pattern of having every day look the same from one to the next, which can be either a pro or a con, depending on your personality and interests. AI physicians continue to face brand new problems and must grow with the ever-evolving field. It can be exciting to be involved in an area of medicine that still has so many unanswered questions, but this can also be overwhelming for people who like clear answers to the problems they face.
You also need to be willing to listen and get curious when something doesn’t check the boxes in the medical textbook. Even years into this practice, you will still encounter once-in-a-lifetime scenarios. Although you train for years to become an expert, the immune system is incredibly complex, and our knowledge about how it works and how it misbehaves is ever-evolving.
And unfortunately, as far as compensation goes, AI is on the lower end. In 2022, AIs made $282,000 a year on average, placing it among the lower third of specialties. However, compared to other IM specialties, AI is ahead of rheumatology, internal medicine, endocrinology, and infectious diseases.
How can you decide if allergy/immunology is right for you?
If you are outgoing, have a deep sense of curiosity, enjoy long, probing conversations, and want to prioritize work/life balance, AI may be the ideal specialty for you.

If you like to have all the answers at your fingertips, get stressed by the unexpected, or enjoy when all the pieces fall perfectly into place, AI may be an overwhelming career path.
In order to succeed, you must be comfortable working directly with patients and seeing patients who are one in a million. You need to be able to distinguish the zebras from the horses because allergists are often asked to weigh in on patients who no one else has been able to figure out.
A career in allergy/immunology is a commitment to lifelong learning.
Are you hoping to become an allergist/immunologist? To get into medical school and match into an internal medicine or pediatrics residency, you’ll need to perform well in school and excel at taking standardized exams. On top of that, you’ll need to craft stellar applications that illustrate your unique story, past adversity, and commitment to medicine.
Med School Insiders has helped thousands of premeds and medical students design their ideal career paths. Our team of physicians has been where you are before, and they’ve become top of their class, attended their dream medical schools, and matched into the nation’s best residency programs. And we’ll show you exactly how it’s done. If you decide on Med School Insiders, we’d love to be a part of your journey to becoming a future physician.
Thank you so much to Dr. Kara Wada, allergist and immunologist based in Ohio for helping with this video. Follow her on Instagram @crunchyallergist.
It’s never too early to begin thinking about the specialty you want to pursue. If you’re struggling to choose the best path for you, our So You Want to Be playlist is a great place to start.

Are you ready to apply to medical school? Use these 6 questions to assess your GPA, MCAT, clinical hours, and application strategy before you submit.

Medical school secondary questions follow predictable patterns. Here are 11 of the most common prompts and how to answer them effectively.
This Post Has One Comment
Thank you for this! Such great help!