
Med School Secondary Application FAQ: 11 Questions Answered
Medical school secondary application FAQs: costs, deadlines, essay prompts, pre-writing strategies, and what admissions committees are actually looking for.
You’ll often hear that internal medicine is for students who don’t know what they want to specialize in, but there are eight subspecialties specific to IM. Here are the main ones for you to consider.

The first is cardiology.
Cardiology focuses on diseases of the heart and vascular system. Cardiologists see many diseases that are quite common, like hypertension, arrhythmias, angina, heart failure, and heart attacks.
To become a cardiologist, you need to finish a cardiology fellowship, which lasts three years. Since this field is so diverse and constantly evolving with new research, you can further subspecialize and train for an additional one to three years.
If you enjoy procedures, you can become an interventional cardiologist, who opens blocked arteries and treats heart attacks. If you like reading ECGs, you can become an electrophysiologist.
The lifestyle of a cardiologist depends on the kind of cardiology practice you want to run. If you want to do procedures, expect to be called in the middle of the night for emergencies. If you want to run a heart failure or electrophysiology clinic, your hours will be much more stable.
Cardiologists are stereotypically extremely confident in themselves, in part because cardiology is the most competitive fellowship in internal medicine. Unsurprisingly, the recently developed Fellowship Competitiveness Index, or FCI, which determines competitiveness based on factors like match rate and salary, places cardiology as the most competitive IM subspecialty. However, full disclosure: This index has not been peer-reviewed yet.
Competitiveness generally follows the money when it comes to medical career paths. Among all IM subspecialties, cardiologists earn the most, with an average yearly salary of $507,000.
To learn more about cardiology, check out So You Want to Be a Cardiologist.
Next, we have gastroenterology.
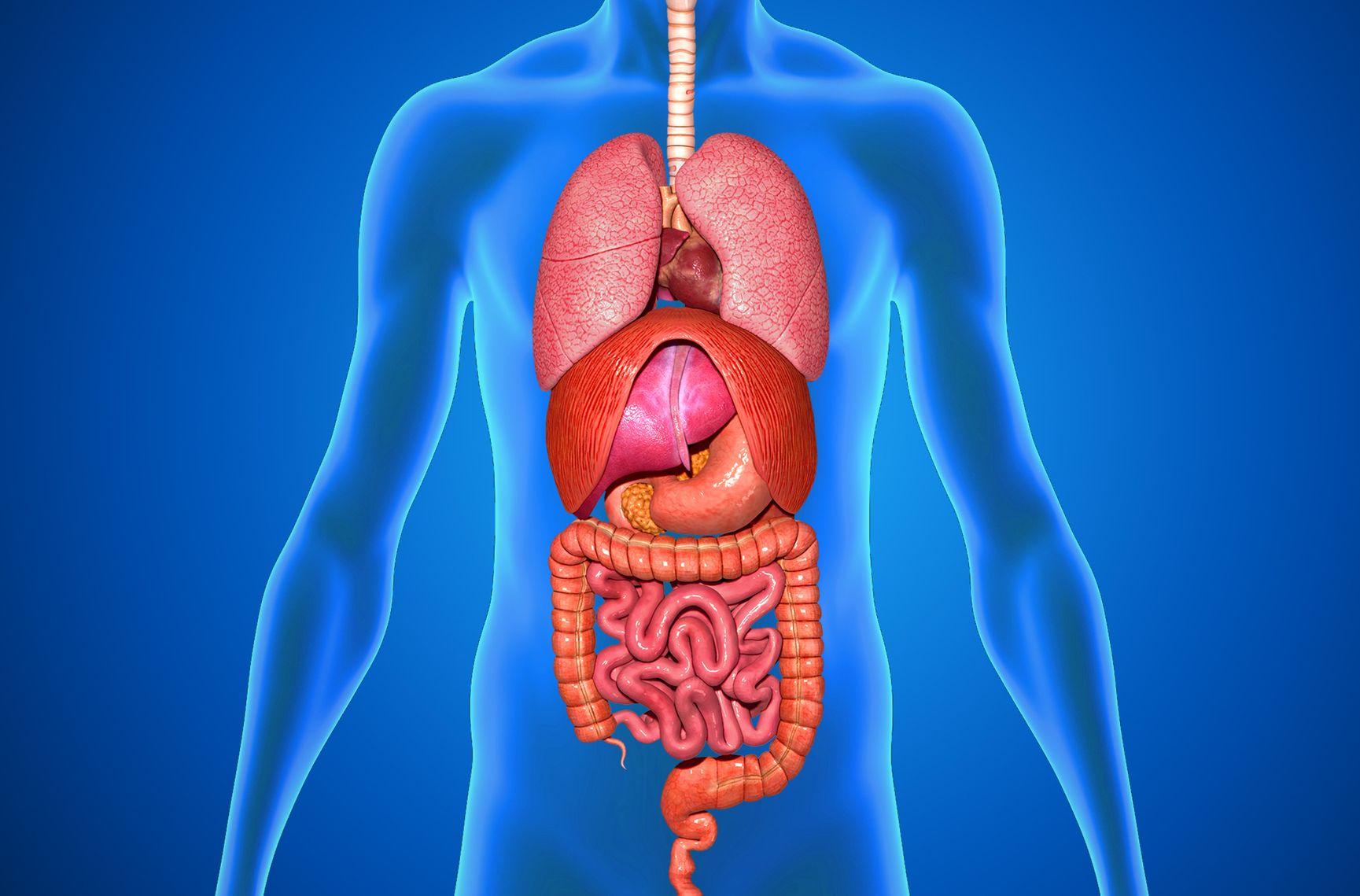
Gastroenterology involves everything in the gastrointestinal tract, ranging from the mouth to the anus and all the internal organs between. You don’t have to like poop to become a gastroenterologist, but you at least have to be comfortable with it.
GIs deal with a wide variety of diseases, including acid reflux, hepatitis, inflammatory bowel disease, irritable bowel syndrome, peptic ulcer disease, and pancreatitis.
Like cardiology, GI fellowships last three years. Afterward, you can choose to practice as a gastroenterologist or pursue additional training, which will also take one to two years, depending on the subspecialty.
You might find yourself leaning more towards liver diseases and assessing patients for liver transplants, or you might prefer procedural work and specialize in advanced endoscopies.
Gastroenterologists can have great lifestyles, but this ultimately depends on your scope of practice. The more time you spend on call or in the hospital on service, the more likely it is you’ll be called for acute emergencies like esophageal bleeds. On the other hand, opening an inflammatory bowel disease clinic is much more stable, and you’ll have a more predictable 9 to 5 schedule.
The FCI places gastroenterology as the third most competitive specialty.
Based on its competitiveness, it’s not surprising that GI is the second-highest-paying subspecialty in internal medicine at an average annual salary of $501,000.
To learn more about gastroenterology, check out So You Want to Be a Gastroenterologist.
The third specialty is pulmonology.
Pulmonary medicine focuses on diseases of the airway, lungs, and chest wall, such as asthma and chronic obstructive pulmonary disease, or COPD. The common stereotype is that if you’re not egotistical enough to become a cardiologist, you’ll become a pulmonologist. This is because there’s a lot of math and physics involved in both fellowships, only with pulmonology, you’re examining air dynamics instead of liquid.
There are two fellowship tracks. The first is pulmonology alone, which lasts two years and is relatively uncommon. The second and more common track is pulmonology and critical care, which lasts three years instead of two.
According to FREIDA, there are 20 pulmonology fellowship programs and 200 pulmonology and critical care fellowship programs.
Critical care physicians treat acutely sick patients and are usually in charge of the intensive care unit, or ICU. The reason pulmonary medicine and critical care are so closely tied is that critically ill patients often need ABC support, standing for airway, breathing, and circulation, the former two of which are squarely in the wheelhouse of pulmonology.
In the ICU, many patients are on ventilators since they can’t breathe themselves, and in these situations, it’s up to pulmonologists to keep the patients alive.
After pulmonology and critical care, you can further subspecialize. If you want procedural work, you can spend a year training in interventional bronchoscopy or right heart catheterization. And if you’re interested in treating patients with obstructive sleep apnea, you can specialize in sleep medicine.
Your lifestyle will depend on your scope of practice. Some physicians prefer running outpatient clinics for asthma and COPD, which can be more laid back. Others prefer to spend more time in the ICU, which translates to more intensity and demanding schedules.
The FCI ranks pulmonology fourth. As for compensation, pulmonary & critical care physicians also rank fourth among IM subspecialties, averaging about $378,000 a year.
If you want to learn more about the day-to-day of a pulmonologist, check out the Day in the Life of a Pulmonary Critical Care Doctor on the Kevin Jubbal MD channel.
Fourth on our list are hematology and oncology.
Hematology focuses on diseases of the blood, like anemias and clotting diseases, as well as cancers of the blood, like leukemia. Oncology focuses on the diagnosis and treatment of cancers.
Hematologists usually see patients with blood disorders in their clinics over time, creating strong patient-doctor relationships. They’re also commonly consulted in the hospital when patients present with complex blood disorders.
Oncologists see cancer patients in their clinics also on a longitudinal basis. They can also work on large, multidisciplinary teams alongside surgeons, radiation oncologists, and more. In the hospital, inpatient oncologists deal with the acute complications that arise from cancer or its treatment.
If you want to individually pursue hematology or oncology, training lasts for two years. However, the more common approach is to train in both specialties, which lasts three years.
Hematologists and oncologists often have a more stable schedule and a better lifestyle compared to the more invasive specialties previously mentioned. That said, urgent issues can come up, so oncologists and hematologists have to be available for their patients.
The FCI ranks hematology-oncology second among internal medicine subspecialties.
As for compensation, heme-onc ranks third among IM subspecialties, averaging $463,000 per year.

Next is rheumatology.
Rheumatology specializes in diseases of the joints, musculoskeletal system, and connective tissue. Rheumatologists see a wide variety of diseases, including autoimmune diseases like rheumatoid arthritis, and musculoskeletal diseases like osteoporosis.
It’s a much more creative specialty. Compared to the straightforward algorithmic management plans of many other IM subspecialties, there’s a lot more gray area in rheumatology.
Rheumatologists practice both in the outpatient setting, where they largely manage chronic diseases, and in the hospital, where they frequently see patients with complex, undiagnosed disorders that may have autoimmune origins. Unlike cards and GI, rheum is not procedure-heavy, as most of the diseases they see are managed with medications.
To become a rheumatologist, you’ll need to finish two years of fellowship training. Physicians also have the option to add an extra year of training to become dual-certified in rheumatology and allergy and immunology.
Rheumatologists have one of the better work-life balances among IM subspecialties. There are very few emergencies for rheumatologists, so you won’t have to worry about being called into work in the middle of the night.
Rheumatology ranked fifth on the FCI, and it’s also on the lower end of compensation, earning an average of $281,000 a year.
Check out So You Want to Be a Rheumatologist.
Sixth is endocrinology.
Endocrinology focuses on diseases of metabolism and the endocrine system, which is made up of glands and the hormones they secrete, including the pancreas, thyroid, adrenals, and many more.
They commonly see diseases like diabetes, hyper and hypothyroidism, and obesity. They also see cancers related to the endocrine system, such as thyroid cancer.
Like rheumatologists, endocrinologists don’t have much procedural work, and their schedule is typically split between the clinic and the hospital.
In the clinic, they follow up with their patients’ hormone labs and treatment responses and make adjustments to their long-term medications, such as insulin. Similar to rheumatology and hematology, these patients stay with you for a long time, so count on building strong patient-doctor relationships.
In the hospital, they’re consulted on patients with endocrine disorders, like hyperthyroidism or metabolic bone disease.
To become an endocrinologist, you’ll have to complete a two-year fellowship after internal medicine.
The lifestyle of endocrinology is similar to rheumatology. There aren’t many procedures or emergencies, so their schedules are more laid back.
According to the FCI, endocrinology ranks sixth out of eight subspecialties, and it’s also one of the lowest-paid, averaging almost $270,000 a year.
Learn more by watching So You Want to Be an Endocrinologist.

The next specialty is nephrology.
Nephro focuses on the kidneys and all that they do. Our kidneys are responsible for many vital functions in the body, such as regulating our electrolytes and fluids, which is an extremely complex process. Nephrologists get even more excited by salt than even IM doctors.
They see a wide range of clinical diseases, including renal failure, acid-base disorders, and hypertension.
In the clinic, nephrologists might see renal failure patients. In the hospital, they are often consulted on patients with acute kidney injury or electrolyte disturbances. They are also often in charge of dialysis units, which help patients whose kidneys aren’t working properly anymore.
To become a nephrologist, you must complete two years of fellowship training. Afterward, you could complete an additional year of training in fields like dialysis or transplant nephrology.
Nephrology is not procedure-heavy and has a stable schedule compared to the more interventional specialties. However, interest in the specialty isn’t as high, and nephrology is the least competitive specialty according to the FCI.
Nephrologists are on the lower end of IM subspecialties, earning around $310,000 a year.
Lastly, we have infectious diseases.
The ID specialty focuses on microorganisms that infect humans, including bacteria, viruses, fungi, and parasites. The COVID-19 pandemic showed the world the importance of infectious disease specialists like Dr. Anthony Fauci—love him or hate him.
Infectious disease specialists focus on complicated or uncommon infections. Not only do they have to know the nature of each disease, but they also have to know the patterns by which these diseases spread across populations, which is why some additionally pursue a Master’s in Public Health.
In clinical practice, ID doctors can work in both outpatient or inpatient settings. In the clinic, physicians can work in more specialized fields like HIV. In the hospital, these doctors consult on patients who have complex infections that don’t respond to normal treatments.
Some specialists also work as infection control specialists or serve on antibiotic stewardship programs to improve hospital antibiotic use.
To become an ID doctor, you must complete two years of fellowship training. Three-year programs also exist for those who want to do an extra year of research and stay in academia. After fellowship, there are opportunities to further subspecialize in transplant infectious diseases or orthopedic infectious diseases.
Regarding lifestyle, there are very few emergencies in this field. Although you might need to be available for your patients around the clock, especially if you’re in private practice or when you’re on call, there aren’t many emergencies that require you to wake up in the middle of the night.
ID specialists often continue practicing well into old age because the work is engaging, not terribly taxing on the body, and you can always step back to part-time.
The FCI places infectious disease as one of the least competitive IM subspecialties, ranking seventh.
One reason may be the low pay, as ID earns the least out of all IM specialists, averaging around $260,000 a year.
To learn more about infectious diseases, check out So You Want to Be an Infectious Disease Doctor.
There are other options for fellowships beyond these eight specialties, but they aren’t specific to IM, which means residents from different specialties might also want to pursue these fellowships. These include adolescent medicine, allergy and immunology, geriatric medicine, hospice and palliative care, and more.
Choosing a specialty is just one piece of the puzzle. Once you’ve decided on your ideal specialty, you’ll still need to match into it.
At Med School Insiders, we have a wide variety of services to help you along the way. From MCAT tutoring to application editing to USMLE prep to mock interviews, we’ve got you covered. There’s a reason we’ve become the fastest-growing company in the space with industry-leading satisfaction ratings. It’s because we deliver results. Period. We’d love to be a part of your journey to becoming a future physician.
If you’re having trouble picking a medical path, check out How to Choose a Specialty in Six Steps.

Medical school secondary application FAQs: costs, deadlines, essay prompts, pre-writing strategies, and what admissions committees are actually looking for.

How many times can you take the MCAT? The AAMC allows up to 7 lifetime attempts, but how many times you should is a different question entirely.
This Post Has One Comment
Please don’t talk behind cardiologists, they are not egotistical