
How Many Times Can (And Should) You Take the MCAT?
How many times can you take the MCAT? The AAMC allows up to 7 lifetime attempts, but how many times you should is a different question entirely.

Contrary to what medical TV shows might have you believe, surgery isn’t just about the surgeon. There is an entire healthcare team behind every surgery that ensures the patient is cared for when they’re under the knife.
Surgery is a fast-moving, complex, multi-faceted aspect of medicine that is deeply dependent on effective teamwork. Without proper respect and communication between all team members, surgery comes to a grinding halt, and the risk of errors and complications shoots up.
Let’s dive into the different parts of the surgical team.
The surgeon is who we most commonly think of when we think of surgery. This is the attending physician who is responsible for the patient, as they made the decision to operate on the patient in the first place, and they are in charge.
Before even getting to the operating room, however, there’s usually significant workup, including labs and tests, that must be performed prior to deciding to operate on a patient. This is obviously not the case with emergency surgeries, such as traumas, but the majority of surgeries are planned in advance. This generally includes a clinic visit with the patient, where the surgeon approaches their concern, performs the appropriate workup, and presents the various options of how to best proceed, often including surgery.
When the patient first comes to the hospital or surgical center and is waiting in pre-op, the surgeon speaks with the patient, obtains informed consent, meaning they again explain the procedure and its possible risks, and answer any questions the patient may have. While they’ve already done this during the clinic visit, doing it again on the day of surgery is essential.
Given that the surgeon bears the weight of the greatest responsibility in the operating room, they are subject to the highest degrees of stress. This is often when you see the stereotypical surgeon personality rear its ugly head. This stereotype is generally “decisive, well-organized, practical, and hard-working, but also cantankerous, dominant, arrogant, hostile, egocentric, and a poor communicator.”

But stereotypes aren’t entirely true, and most surgeons I know don’t fit the mold in terms of these negative qualities. I would say, however, that most surgeons I know are more direct, efficient, and pragmatic than most and perhaps not afraid to be rough around the edges in order to get the job done.
Some studies have concluded the surgical personality certainly does exist, but they instead highlight their novelty-seeking, competitive nature and reward-dependent qualities, in addition to scoring higher in self-discipline and achievement but lower in compliance and vulnerability.
If you think you might be interested in becoming a surgeon, check out our So You Want to Be a Surgeon specialty breakdown.
At teaching hospitals, the surgeon enters the operating room once the patient is under anesthesia and ready to be operated on. They may have their residents drape, but many surgeons are highly particular and prefer draping the patient themselves. The surgeon performs the surgery and must remain by the patient’s side until they are extubated, meaning the breathing tube is removed, and they are wheeled out to post-op.
The surgeon operates in a sterile field to minimize the risk of surgical infections. On the other side of the drape is the anesthesiologist.
Think of anesthesiologists as the guardian angel for the patient as they approach a scary time in their life.
The anesthesiologist is the other attending physician in the room and can generally be thought of as second in command. But don’t tell any anesthesiologists that. The surgeon is the captain of the ship, but the anesthesiologist is right by their side. That doesn’t mean their job isn’t equally foundational.
Just like the surgeon, the anesthesiologist will visit the patient in pre-op, but rather than the procedure, they’ll be focusing on explaining how they’ll keep the patient comfortable during the case. This often includes general anesthesia, where the patient goes under and requires a breathing tube.
However, anesthesiologists can also provide sedation, where the patient is deeply sedated and doesn’t remember the procedure, but they’re able to breathe on their own. Local or regional anesthetic doesn’t interfere with the patient’s consciousness, but rather numbs the area that the surgeon will be working on.
Prior to the case beginning, the anesthesiologist provides the appropriate anesthetic to the patient. This may include providing certain pre-op medications via IV and intubating the patient if they’ll receive general anesthesia.
During the case, they monitor the cardiopulmonary status of the patient, ensuring they’re safe and comfortable. This is done through cardiac leads on the patient’s skin to monitor heart activity, a pulse oximeter on the finger to monitor oxygen saturation of the blood, and a blood pressure cuff to monitor circulation.
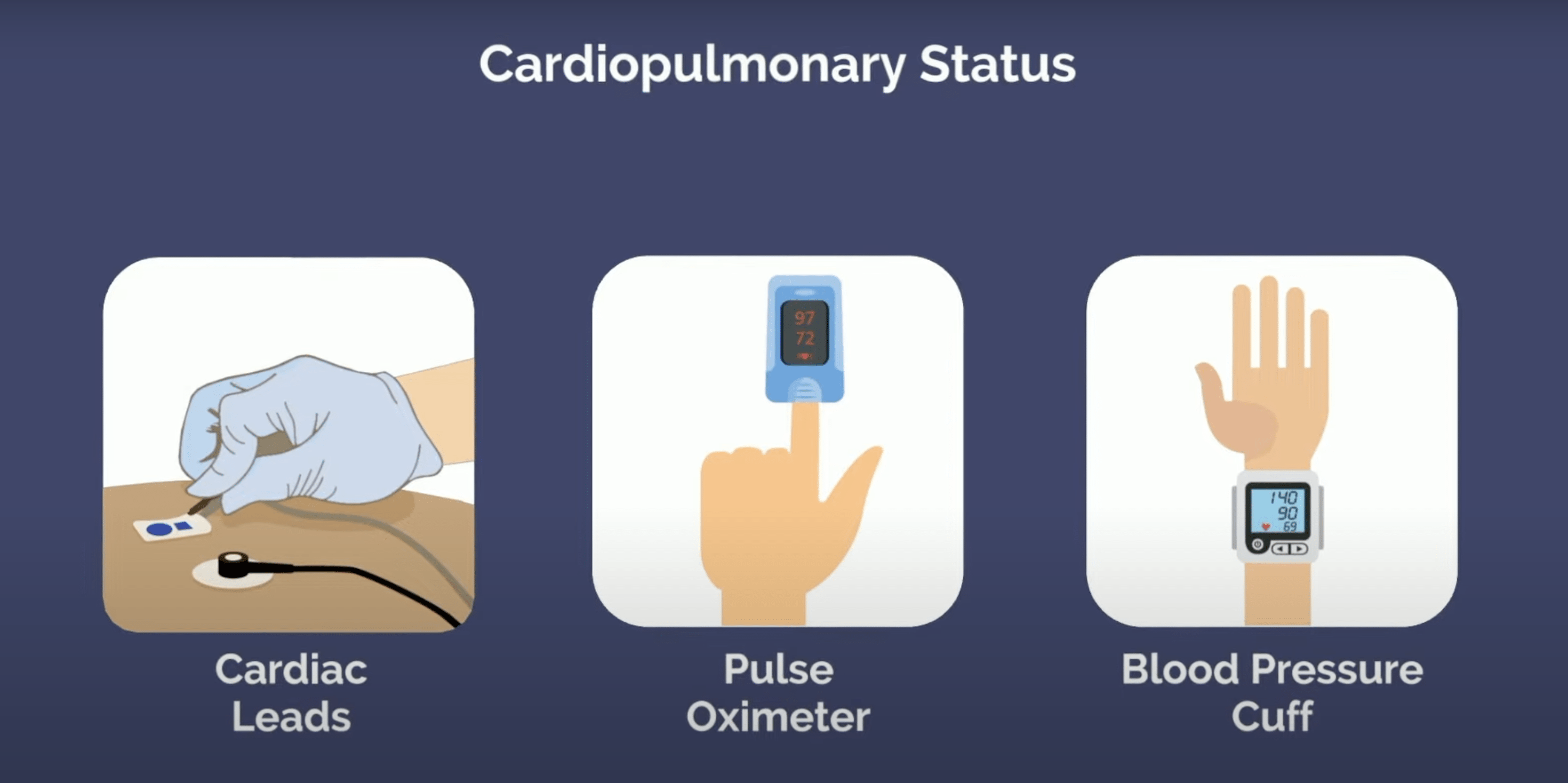
After the surgery, they’ll reverse the analgesics, and once the patient is stable, wheel them to post-op and hand them off to the nurse in the post-anesthesia care unit, or PACU.
If you’re interested in becoming an anesthesiologist, check out our So You Want to Be an Anesthesiologist specialty breakdown.
The surgical first assist is the person helping the surgeon perform the case, who is also scrubbed into the sterile surgical field. This is most commonly a resident, physician assistant (PA), nurse practitioner (NP), certified surgical assistant (CSA), or medical student. It’s their responsibility to assist the surgeon in performing the procedure, which includes a lot of retracting, suctioning, and performing other supportive measures for the surgeon.
Being a good first assist requires knowledge of anatomy and physiology, surgical handling of tissues, understanding surgical instrumentation and its use, and the nature of the procedure.
The first assist should also be skilled in suturing, positioning, sterile technique, prepping and draping, and the use of splints and casts. Things generally go smoother when they’re also highly perceptive and have a strong intuition when it comes to predicting the needs of the surgeon.

The scrub nurse is also scrubbed in the surgical field and is the one preparing, organizing, and providing the various surgical tools and instruments to the surgeon and first assist during the case.
While that may sound simple, it’s extremely fast-paced, demanding, and requires a similar understanding, perception, and familiarity as a first assist to keep things moving smoothly. A guaranteed way to annoy a surgeon and increase tension in the room is to keep them waiting longer than needed for the necessary instrument.
Prior to the case beginning, the scrub nurse gathers the necessary supplies, including the sets of surgical instruments needed for that particular type of procedure. They’ll be the first one to scrub in and set up a sterile surgical field for others to join, helping the surgeon and assistants with their sterile gown and gloves.
The scrub nurse is critical to things moving smoothly and is one of the primary drivers in anticipating the needs of the surgical team.
The circulator is the point person in helping assist the surgical team outside of the sterile surgical field. Along with the scrub nurse, they are also responsible for gathering supplies, sterile equipment, and toolsets needed for surgery and anesthesia.
They also manage the documentation at the computer before and during the case, including verifying the patient’s ID, who all is in the room, getting the patient comfortable with warming blankets, and the like. Together with the scrub nurse, they’ll help the surgeon and assistants get gowned in a sterile fashion, and it’s common for them to also help prep the surgical site with washing agent and other prep materials.
During a case, they’ll grab additional supplies as needed and help out the surgical team, who cannot leave the sterile field. Toward the end of the case, they’ll ensure an accurate count of sutures, needles, sponges, and lap pads. You don’t want to accidentally leave a sponge or needle in a patient—and yes, it happens. They’ll help apply dressings and get the patient safely transferred to the PACU.
In addition to the core team, you’ll often see medical students or residents in surgical cases at teaching hospitals. Junior medical students generally observe, doing their best to stay out of the way and, of course, not contaminate the sterile field. If they’re scrubbed in, they may be retracting, suctioning, and essentially learning the ropes as a first assist.
Medical students who are deliberate in applying themselves will also earn the right to close, meaning suture the incision shut at the end of the case. Closing the superficial layers, such as the skin, is easier and lower risk, so attendings are more willing to hand out that responsibility. Closing deeper layers, however, requires that the attending trusts you due to the added complexity and risk if poorly executed.

The responsibilities and tasks of a resident will be highly variable depending on their year in training and the institution.
Junior residents serve as the first assist at the minimum but, depending on their skill level and aptitude, may be granted substantial responsibility in helping with various aspects of the case. After all, this is how attending surgeons are made—they must learn in residency.
Senior residents take on additional responsibility and generally take ownership of the case, performing the majority themselves with oversight from the attending. They will soon be out in the world as attendings themselves, handling cases on their own.
There are several other key members who are directly related to surgery that don’t step foot in the operating room.
The OR supervisor manages all operating theaters, ensuring things run smoothly. They book and schedule cases, assign rooms, and act as a coordinator between the preoperative holding area, OR, and PACU.
The preoperative holding nurse preps the patient before the case, checking them in, organizing consent, notes, and orders. They also check vitals, start the IV, and administer medications.
The PACU or recovery room nurse accepts the patient from the OR and provides a secure environment for recovery.
There may be additional team members in the OR, depending on the case or the institution.
Surgical techs provide further assistance and are key in preparing the operating room, tools, and equipment. Medical device reps in the OR help the surgeon use their company’s devices properly. CRNA’s provide anesthesia under the anesthesiologist’s supervision.
Together, all parts working in harmony translate to a successful and nearly seamless experience for the patient. It’s not about you or your ego or who said what or whose toes were stepped on. And at the end of the day, it’s all about the patient.
Which surgical team role most resonates with you? Let us know with a comment down below.
If you’re unsure what specialty is right for you, check out our So You What to Be… series, which provides insight into what it’s like to pursue different specialties. We have dozens of articles and corresponding YouTube videos. If you don’t see a specialty you’re interested in, leave a comment below to make a request.

How many times can you take the MCAT? The AAMC allows up to 7 lifetime attempts, but how many times you should is a different question entirely.

How many times can you apply to medical school? Learn the limits, what’s actually advisable, and what to do if medicine doesn’t work out.